About Health Inequalities
Europeans consistently say that health is one of the most important issues to them 1Standard Eurobarometer; https://ec.europa.eu/commfrontoffice/publicopinion/index.cfm. The past few years have shown how central health is to our economies and societies. From the COVID-19 pandemic to rising challenges like mental health, chronic illnesses, and climate-related health risks, it is clear that some groups are much better equipped to protect their health than others.
What are health inequalities?
Health inequalities are the ‘systematic differences in health between social groups’ that are avoidable and unfair. Find a full definition in the health inequalities glossary.
The higher a persons’ socio-economic status the healthier they are likely to be. This is the case in all regions of the EU. Income or educational level usually determines socio-economic status.
A person’s, socio-economic status compared to others living in the same place reflects their relative likelihood of:
- becoming prematurely ill
- being overweight or obese
- dying prematurely.
Recent health crises have not only brought existing health inequalities into sharp focus. In some cases it has increased them, through its disproportionate impact on certain population groups.
Health inequalities are evident amongst people in different income, wealth, and educational groups but also amongst people of different genders, race and ethnicities, occupations, and areas of residence.
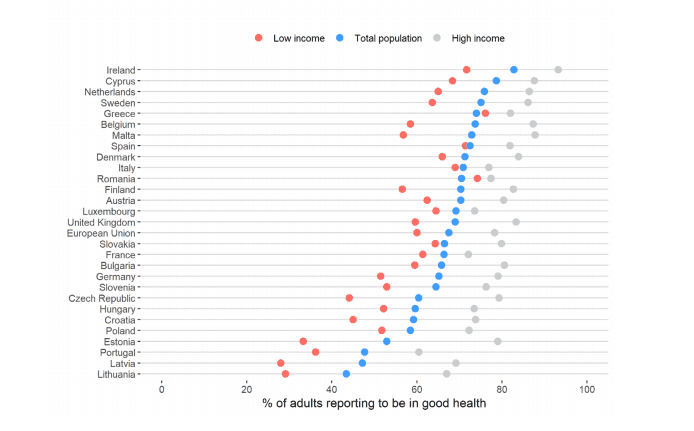 Disparities in self-reported health by income (Forster, T., Kentikelenis, A., Bambra, C.; Health Inequalities in Europe: Setting the Stage for Progressive Policy Action; https://doi.org/10.13140/RG.2.2.20665.21608)
Disparities in self-reported health by income (Forster, T., Kentikelenis, A., Bambra, C.; Health Inequalities in Europe: Setting the Stage for Progressive Policy Action; https://doi.org/10.13140/RG.2.2.20665.21608)
Who is affected?
Health inequalities affect everyone. The 'social gradient' or the 'socio-economic gradient in health' demonstrates this. The term social gradient describes the phenomenon that for every step down the socio-economic ladder there is a corresponding decrease in health status. In other words, the greater the level of disadvantage, the poorer the state of health and the shorter the life expectancy. This correlation is apparent in all societies.
How can you measure differences in health status?
We measure differences in health status by:
- mortality,
- morbidity (incidence of disease)
- how likely people are to engage in behaviours that pose a risk to health. Those can be behaviours like smoking, excessive consumption of alcohol, insufficient exercise, or bad diets..
Are health inequalities avoidable?
The steepness of the health gradient and the level of inequalities varies between countries and regions. This shows that:
- they are socially constructed
- they can be reduced by reasonable means
- that they are therefore avoidable and unfair.
More information on health inequalities and the socio-economic gradient in health, with specific figures from across the EU can be found in this factsheet.
80.4% of the richest 20% of the population in the EU consider themselves to be in good or very good health, compared to 61.2% of the poorest population.
Self-perceived health of the bottom 20% of the poorest population compared to the average population and the top 20% of the richest population. Taken from the EuroHealthNet factsheet on health inequalities.
Health inequalities and COVID-19
 The CHAIN infographic illustrates that COVID-19 is in fact a syndemic pandemic (link)
The CHAIN infographic illustrates that COVID-19 is in fact a syndemic pandemic (link)
It is predicted that the COVID-19 pandemic will lead to economic recession across Europe, which will exacerbate health inequalities. It is becoming increasingly evident that those in lower income groups, and low skilled employment are most likely to catch and die of the disease. The COVID-19 pandemic will exacerbate those pre-existing health inequalities, and have the heaviest impact on the lives of people living in deprivation. The limited data already available (from the UK) suggests that low skilled men have the highest death rate among working age adults. Further research suggest that Black males and females are 4.2 and 4.3 times respectively more likely to die from a COVID-19-related death than White ethnicity males and females. It seems that most fatalities are amongst those with underlying illnesses such as high blood pressure, diabetes and heart or respiratory disease 2Hans Henri P Kluge, *Kremlin Wickramasinghe, Holly L Rippin, Romeu Mendes, David H Peters, Anna Kontsevaya, Joao Breda; Prevention and control of non-communicable diseases in the COVID-19 response; https://doi.org/10.1016/ S0140-6736(20)31067-9 3 Martini N, Piccinni C, Pedrini A, Maggioni A; CoViD-19 and chronic diseases: current knowledge, future steps and the MaCroScopio project; Recenti Prog Med. 2020 Apr;111(4):198-201. doi: 10.1701/3347.33180; https://www.ncbi.nlm.nih.gov/pubmed/32319439 4 Wang B, Li R, Lu Z, Huang Y; Does comorbidity increase the risk of patients with COVID-19: evidence from meta-analysis;Aging (Albany NY). 2020 Apr 8;12(7):6049-6057. doi: 10.18632/aging.103000. Epub 2020 Apr 8.;https://www.ncbi.nlm.nih.gov/pubmed/32267833.
The more socially and economically disadvantaged a person is, the more likely they are to suffer from these diseases. Diseases that are largely preventable. The spread of the virus has highlighted the needs of migrants, asylum seekers, and Roma people who already experience discrimination and health inequalities. They make up just some of the 26% of people in Europe living in overcrowded spaces. In confinement, people are more exposed to interpersonal violence at home – notably women and LGBTI people.
Mental Health
This social gradient also applies to risks of mental ill-health, which will be exacerbated by isolation, fear, and insecurity. A survey from the Netherlands National Institute for Public Health and the Environment found that more than a third of people say they felt much more anxious, despondent, stressed and lonely during the pandemic. About 20% are having more problems sleeping than before. In France, a survey from the public health institute found that 27% survey respondents reported a state of anxiety; the factors contributing to this feeling include being in an unstable financial position, having a poor understanding of transmission of the virus, feeling of being ill-equipped to adopt to recommended measures, and having little confidence in public authorities. People in deprived areas are less likely to receive treatment for mental ill-health 5In 2018, 26.2% of the European population with an income below 60 % of median equivalized income lived in overcrowded dwellings. Overcrowding rate by age, sex and poverty status – total population – EU-SILC survey 2018.
Why is it important to address health inequalities?
For individuals
Inequalities in health reflect how large numbers of people are being denied the resources for health and additional years of life. Health allows people to participate in social and economic activities. It is key to a person’s well-being, happiness, and satisfaction. People who are physically, mentally, and socially well are more likely to perform better academically and in the workforce. They are also more likely to avoid poverty.
For societies
Health inequalities also undermine societal well-being. For example, high levels of health inequalities put a greater demand on health care systems and other areas of public spending. Researchers have found that inequality reduces social cohesion, which leads to more stress, fear, and insecurity for everyone. More socially cohesive, educated populations by contrast are likely to have lower rates of crime and civil disorder and more highly skilled workforces.6Wilkinson, R., Kate Pickett, K. The Spirit Level: Why More Equal Societies Almost Always Do Better. Allen Lane, 2009 Levels of health inequalities serve as a good indicator of whether economies are succeeding in generating well-being. They show whether the economy is contributing to what all citizens consistently indicate that they value most –their health.
 Adapted from Baum, F. E.; More than the tip of the iceberg: health policies and research that go below the surface; https://doi.org/10.1136/jech.2009.091595
Adapted from Baum, F. E.; More than the tip of the iceberg: health policies and research that go below the surface; https://doi.org/10.1136/jech.2009.091595
What are the causes of health inequalities?

Complex and interlinked factors cause Health inequalities and the social gradient. They fundamentally result from socio-political factors that lead to differences in the distribution of power, money and resources between different population groups and social classes. These, in turn, result in differences in environmental and individual resources. Those resources are, for example, the quality and availability of employment, housing, transport, access to services, and social and cultural resources. Such resources are also referred to as determinants of health, because they affect opportunities for good health, and how people think, feel and act.
- the quality of care that an infant or child receives
- whether a person has sufficient income to meet their basic needs
- their employment status and conditions
- the quality of their housing and communities are all.
These factors affect whether individuals have the capacity, the opportunity or the motivation to, for example, eat well or to get adequate physical activity. They also determine if a person has access to quality treatment and care when illness occurs, and the ability to benefit from this.
5 contributing factors
WHO Europe has identified five conditions that contribute to health inequalities in self-reported health, mental health, and life satisfaction. The WHO Health Equity Status Report indicates that 90% of health inequalities can be explained by these 5 factors:
- Quality of health care.
- Financial insecurity.
- Poor quality housing and neighbourhood environment.
- Social exclusion.
- Lack of decent work and poor working conditions.
In recent years it has also become clear how levels of health inequalities are related to production and consumption patterns, particularly in highly industrialised economies like those in the EU. The destabilisation of the environment has grave repercussions for health and well-being. The effects of environmental degradation and climate change will ultimately affect the health and quality of life of everyone. However, they have a disproportionate effect on those who are already more vulnerable.


